Blog: Documenting rural heat health disparities in the U.S.
Published: April 1, 2025
…
Rising temperatures and extreme heat events—which are becoming more frequent and intense due to climate change—pose serious health risks. Most research on the health impacts of heat focuses on cities, where dense populations and the urban heat island effect make heat impacts more visible. As a result, the effects of extreme heat on rural communities have been largely overlooked.
In our newly published study in The Journal of Climate Change and Health—Rural heat health disparities: Evidence from the U.S. National Emergency Medical Services Information System (NEMSIS)—we analyzed national emergency medical services (EMS) response data to compare heat-related illness (HRI) cases in rural and urban areas across the U.S. Our research looks at how patients in both settings fared after an EMS response, shedding light on rural heat risks.
Key Findings
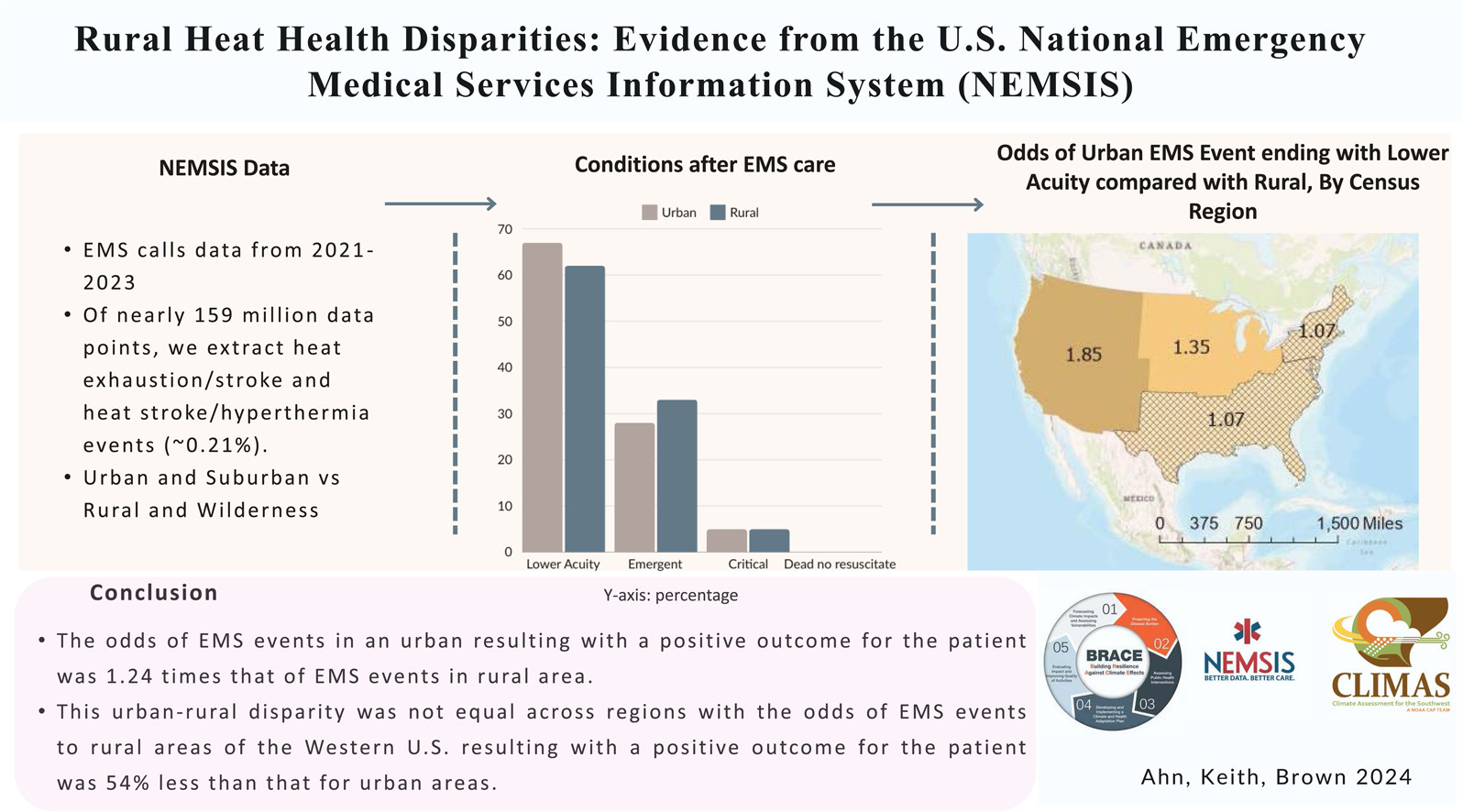
- Our study found that patients in urban areas were more likely to end their EMS trip with a lower-acuity outcome compared to those in rural areas (Odds Ratio: 1.24, 95% CI 1.13-1.36) for heat-related illness (HRI) emergencies.
- When broken down by region, the gap between urban and rural HRI outcomes was most pronounced in the Western U.S.
- As expected, emergency response times were longer for rural areas, with a median delay of 2.1 minutes from unit dispatch to patient arrival.
Notes for the analysis
- We defined urbanization at the county level, and this study reclassified ‘Urban’ to include urban (83.7% of events) and suburban (6.6%), and ‘rural’ to include rural (8.0%) and wilderness (1.8%).
- We categorized regions based on U.S. Census definitions: West, Midwest, South, and Northeast.
- All events identified as HRI data including heat stroke/exhaustion and heatstroke/hyperthermia between 2021 and 2023 were included.
- Our dataset included all HRI-related EMS events from 2021 to 2023, including cases of heat stroke/exhaustion and heatstroke/hyperthermia.
- Since HRI cases are often underreported or misclassified and coded as something other than HRI, we acknowledge this limitation in our dataset, as seen in other studies.
Significance
Our analysis systematically demonstrates with nuance that, in the U.S, rural regions tend to have worse HRI outcomes than urban regions despite the focus on urban heat. This difference is more pronounced in the Western U.S. than other regions.
To fully understand and address these disparities, we need better data collection and further research. We hope our findings encourage key stakeholders to prioritize rural heat resilience and improve health outcomes for those most at risk.